Key Takeaways
|

As we face the current global pandemic from COVID-19, many world leaders are stating that they are fighting two wars. One is an epidemic prevention war to avert the healthcare systems from collapsing under a surge of infections and critical illness, leading to dramatic rises in mortality and morbidity (War 1), and the other is the war to save the economy from being strangled by stringent public health measures leading to global recession (War 2). The two wars are almost perfectly negatively correlated in terms of infected cases vs. the economic costs.
These leaders are setting up ‘War cabinets’; putting their nations on a “War Footing”. There is even one leader who calls himself a “War-time President”.
In a conventional war, Generals start calculating how many of their soldiers they are willing to sacrifice to hold off the enemy until the cavalry arrives. This may eventually be the reality for all governments in these two concurrent wars. They will need to consider how many human lives they would need to sacrifice to both prevent the health system from being overwhelmed and simultaneously sustaining some semblance of the economy – until a vaccine or cure arrives.
To fight both wars, predictive information is required so that the leaders and their advisers are not making decisions in a vacuum. This requires both epidemiological and economic modelling.
Epidemiological Modelling (To Fight War No.1)
The basic argument put forward by public health specialists advising governments is to “flatten the curve”. This has rapidly become a rallying cry in the fight against COVID-19, popularised by media outlets and leaders worldwide. The COVID-19 “flattening the curve” infographic (Figure 1), put out by the Centres for Disease Control and Prevention has entered our collective consciousness worldwide (Economist, Feb 29, 2020).[i]
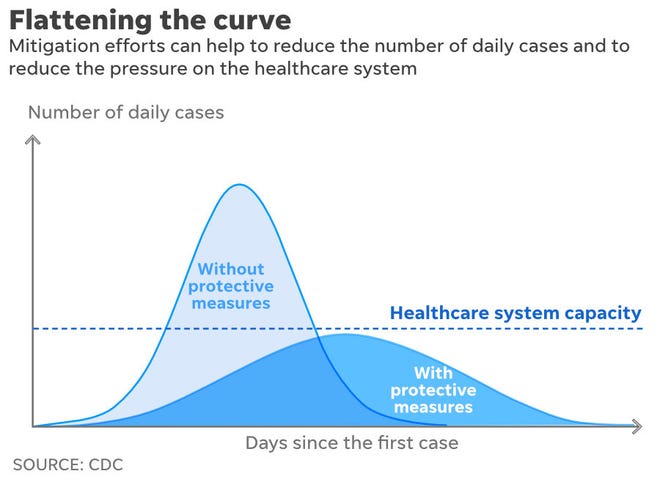
This approach advocates a number of interventions – such as strict personal hygiene, social distancing, case isolation, contract tracing etc – aimed at slowing the progression of the virus through the community, such that the number of people unwell and requiring hospital care at any one time does not overwhelm the health services’ capacity to treat them.
There is much global uncertainty and contention at how best to “flatten the curve”, including timing of interventions, who should be subject to restrictions and for how long these should be imposed. Most importantly, its unknown how successful they will be. Figure 2 shows the modelling done by Professor Neil Ferguson at the MRC Centre for Global Infectious Disease Analysis at the Imperial College, London. In this graph, the red flat line assumes no change in the number of intensive care unit (ICU) beds in the short-run (Ferguson, et. al., 2020).[iii]
The aim of mitigation is to use nonpharmaceutical interventions or NPIs (and vaccines or drugs, if available), not to interrupt transmission completely, but to reduce the health impact of an epidemic. In this scenario, population immunity builds up through the epidemic, leading to an eventual rapid decline in case numbers and transmission dropping to low levels.
The aim of suppression is to reduce the reproduction number (the average number of secondary cases each case generates) to below 1; and hence to reduce case numbers to low levels or ideally to eliminate human-to-human transmission. The main challenge of this approach is that NPIs (and drugs, if available) need to be maintained – at least intermittently – for as long as the virus is circulating in the human population, or until a vaccine becomes available.
Figure 2 shows that currently in the UK, there are less than 10 ICU beds per 100,000 of population. As the population of the UK is approximately 70 million, this would mean that, based on Figure 2, the UK has approximately 5,600 ICU beds (or 0.008%). Villa (2020) states that the USA has 95,000 intensive care beds for a population of 330 million people (0.03%). From an article by Hicks, et. al. (2019), it can be ascertained that Australia has about 2,000 ICU beds for its 25 million population (or 0.008%), the same as the UK.[iv]
Figure 2 indicates that the curve with the highest peak is if the government does nothing and allows society and the economy to function normally. In such a scenario, the critical care bed capacity that the UK will need is about 280 ICU beds per 100,000 of population. The curve with the flattest peak is one involving case isolation, home quarantine, and social distancing of the over 70s only. In such a situation the UK will only need to increase its critical care bed capacity (i.e. make more ICU beds) to about 100 ICU beds per 100,000 of population, which still reflects a 900% increase in capacity.
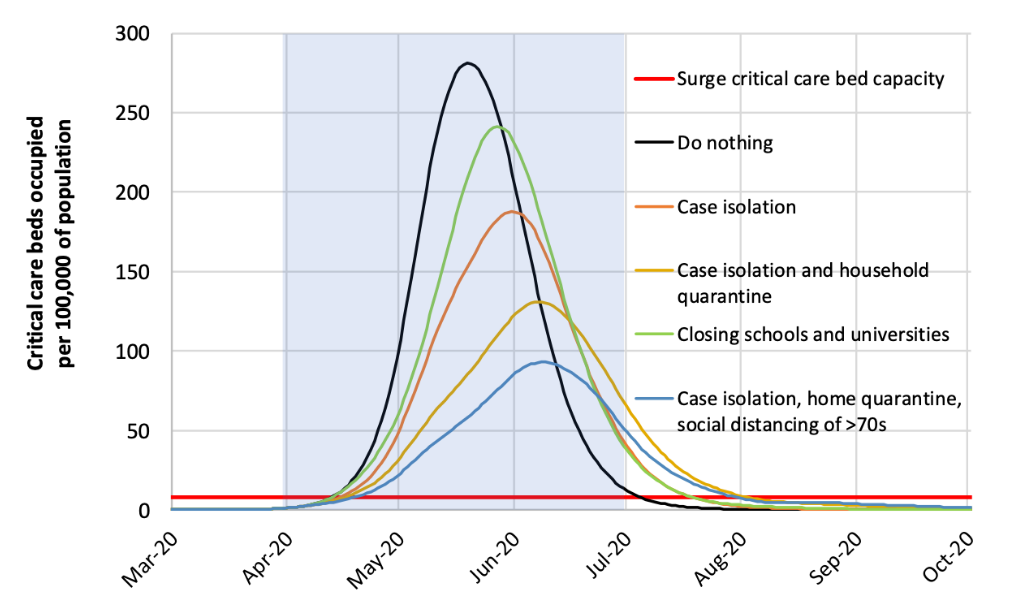
Whilst this may be possible in a developed country on a war-footing, it will still mean a significant number of infections, and related deaths. Therefore, even more, stringent social distancing measures may need to be applied to slow the infection and save lives. This could only come at an enormous economic and social cost.
Therefore, assuming that the epidemiological trends forecast in Figure 2 can apply to other countries; the governments of those countries will need to make some hard decisions. Either they fight it hard now to suppress the spread and avoid a massive epidemic in which hundreds of thousands – if not millions, in poorer countries – will die, or they prioritise the economy and ‘let nature take its course’ via mitigation.
Unfortunately, even in countries that decide to fight hard, Figure 2 shows that moderate restrictions (i.e. case isolation, home quarantine, mask wearing, and social distancing of the over 70s only – especially those in aged care homes) will not be enough to prevent the health system from being overwhelmed. As such, few countries have decided not to fight hard. Sweden, for example, has adopted a relatively relaxed strategy when compared to its Nordic neighbours, seemingly assuming that overreaction is more harmful than under-reaction (Franks & Nilsson, 2020).[v] Brazil’s President Jair Bolsonaro calls the pandemic a ‘momentary little flu’ and asserts that Brazilians have ‘natural immunity’. Only time will tell which approach is most successful and at what costs.
Is This Increase in Capacity Financially Viable?
We have already shown that the UK health system would need an increase in capacity of 900% from the present 10 ICU Beds per 100,000. The USA health system, despite having a much better ratio of ICU Beds per population than the UK or Australia, will still need about 330,000 ICU beds for its total population, an increase of about 250%.
For Australia, this would mean an extra 20,000 ICU beds for 2 months, an increase of 900%, just to meet the peak under the moderate restrictions as per Figure 2. In 2019, the estimated total annual operational cost for ICU care in Australia was $2.1 Billion for 2,000 ICU Beds; about 0.15% of gross domestic product (GDP) and 1.4% of total health care costs (Hicks, et.al, 2019). Working from these annualised numbers, it works out to over $1 million per year per bed or approximately $3,000 per bed per day. However, Hicks, et.al, 2019 have also stated in their paper that the mean cost per patient bed‐day for all contributing ICUs was $4375, with a standard deviation of $1157.[vi]
Let us say, for argument’s sake, that today’s costs are $5,000 per bed per day. An extra 20,000 ICU Beds for 2 months would cost the government approximately $6,000 million or $6 Billion.[vii] Let us now double that figure to $12 Billion to account for capital expenditure, organisational overhead costs, and equipment costs. Given that the Australian Federal Government is spending 130 Billion to keep the economy in ‘hibernation’ for 6-months (discussed later) this level of expenditure will be comparatively miniscule; especially if the private hospitals and hotels are ‘commandeered’ into the war effort.
Figure 2 indicates that the current level of suppression would still mean a significant number of infections, but spending $12 Billion on providing a full capacity number of ICU Beds for 3-months will get the health-care system over the peak, and significantly reduce patient deaths. As such, there does not appear to be any reason, hospital capacity wise, to ‘hibernate’ the economy for more than 3-months.
After this period, a targeted suppression approach could be implemented to protecting the most vulnerable, whilst keeping the economy running (also discussed later). The Australian Federal Government can save at least $65 Billion by not ‘hibernating’ the economy for a further 3-months. This will not only save the economy and prevent global recession and its sequalae, which could include significant health impacts (Collins and Cox, 2020).[viii]
It must also be remembered that these financial modelling cost estimates are changing daily and the $5,000 per bed per day may be an over-estimation. An MIT team has just announced that they have developed a cheap, open-source ventilator called the MIT E-Vent that could get regulatory approval soon (Chandler, 2020).[ix] On the same day as the MIT announcement, it was announced that Australia’s first ‘virtual hospital’ for COVID-19 patients will be established within two weeks to treat coronavirus patients from their homes. Hundreds of coronavirus patients who are present at the Armidale Hospital emergency department in the far north of NSW – and who otherwise would have needed a hospital bed – will soon be allowed to go home with sophisticated machines to monitor their vital signs (Mannix, 2020).[x] It is entirely possible that such ‘virtual hospitals’ will be monitored on a 24/7 basis using subcontracted Indian medical specialists residing in India.
With the promise that such new innovations, testing regimes, vaccines and other treatments will be available before the economy goes into recession (and even depression), many Western countries, and some Asian late-movers, are electing to fight hard. They are imposing very strict quarantine and social distancing measures on all inhabitants regardless of their age; rather than only on those most vulnerable to the effects of the virus and most likely to need intensive hospital care. This is the Wuhan total lockdown model, but it will come at a massive economic cost. Already we are witnessing worldwide the unprecedented economic and social impacts of social distancing measures that range from curfews, border controls, lockdowns, and the like. The economic modelling of the impact of such a lockdown will be discussed later.
The Australian government has chosen to fight hard by imposing with the threat of fines, the maximum restrictions on the population that a democracy will accept. The hope is that with extreme social distancing measures, we can buy time to build our armies – in workforce capacity, protective equipment supplies, infrastructure and treatments – to be better prepared for the inevitable war ahead.
The Economic Paradox
Although nobody has innate immunity to this animal-borne virus, the one thing most people know about COVID-19 is that it is most lethal in older people. The data from around the world clearly indicates that Seniors age group (70 years old and older) are the most likely to be hospitalised; and that a significant percentage of them will ultimately die (Scott, 2020).[xi] Many of those over 80 years and over would be in aged care facilities that would need particular protection. Hired nursing and other staff may be much more likely introduce the virus to the facility; rather than any potential contamination from visiting family members. A single contaminated member of the care facility staff would quickly become a super-spreader throughout the entire facility, and beyond.
We also know from the data that people who have underlying medical conditions, particularly those with heart disease, diabetes, high blood pressure, lung disease, and cancer; face higher odds of getting really sick or dying from COVID-19. Having one or more of those conditions increases a person’s risk of severe symptoms beyond what their age alone would suggest.
The economic paradox is that the casual workers who are the hardest hit by these draconian economic shutdown measures tend to be of the younger age groups in which COVID-19 has had the least impact worldwide in terms of severity requiring hospitalisation. Conversely, the group most likely to require intensive care hospitalisation is the one that is least affected by social distancing laws; i.e. the seniors who are mostly retired, stay mostly at home and are not dependant on an hourly wage (Scott, 2020).[xii]
However, most governments, quite rightly, are not discriminating when they apply the new social distancing and lockdown laws by age or medical condition. Everyone is asked to stay at home as much as practicable, and those with the symptoms and those who have tested positive to COVID-19 are asked to strictly self-isolate at home. Only the very serious cases will be admitted to the hospital.
In normal hospital practice, medical professionals routinely make judgements and recommendations about which treatments may be effective for patients and which may be futile, based on their health status, personal values and available resources. Patients and families are usually heavily involved in these decisions. In the current pandemic crisis however, as we have seen in neighbouring countries like Italy and Spain, hospitals are operating more like battlefields – with doctors having to make rapid decisions about likelihood of survival and rationing ICU beds and lifesaving treatments like mechanical ventilation only for those most likely to survive. Patients that would have ordinarily been treated, and potentially survived, are being automatically denied access to treatment based on demographic and medical factors and death tolls are mounting. These life-and-death decisions are taken away from the affected individual or their family.
Rather than forcing rapid life-and-death decisions of patient care and resource allocation to be made by medical professionals at the frontline, governments should explore options to reduce the burden of end-of-life decision making prior to hospital arrival. For example, governments could offer financial support and lodgings to those who cannot quarantine themselves safely or effectively at home. Many older people with multiple medical illnesses living with constant disability do not want any life-saving measures to be performed for them if they were to become critically unwell.
Governments should widely educate and empower people to formalise their wishes about end of life care within legal documents known as ‘Advanced care directives’ so that their wishes can be upheld in these circumstances without anguish from doctors and family. It may also be time to revisit the highly emotive Voluntary Assisted Dying laws (temporarily) to give some of the choices back to the individual; so that they could, if they wish, be assisted to die under medically controlled conditions; rather than be subject to months of isolation or die after suffering. GPs should also be urgently trained to oversee such procedures in patients’ homes to reduce hospital burdens.
Could Economic Incentives Have a Role?
This is a period of absolute crisis where governments and the medical profession will be struggling to conserve scarce resources. Perhaps economic theories and principals can assist in streamlining some of these decisions. In economics, there is a valuation method called ‘Contingent Valuation’; which is a method of estimating the value that a person places on a good. The approach asks people to directly report their ‘willingness to pay’ to obtain a specified good, or ‘willingness to accept’ to give up a good, rather than a third-party inferring them from observed behaviours in regular market places.
Monetary incentives or influences within health decisions are not new concepts. Examples of monetary drivers include withholding of medical services due to lack of health insurance, as in the USA; or conversely excessive testing and treatments for futile or unnecessary conditions in those who can simply afford to pay for it. In the extreme circumstances we find ourselves in, Governments may need to consider extreme measures, including the contingent valuation approach on human lives. Well people could be financially incentivised to remain at home in strict lock-down, or more perversely, people could elect to receive a payment or life-insurance payout instead of receiving hospital-based care if they became unwell.
The aim would be to match available hospital resources with those who would benefit and want the treatment- though a plethora of legal, ethical and moral implications would need to be addressed. Whilst, a layperson can ask someone directly what monetary compensation he or she is ‘willing’ to accept to give up their life, they cannot legally be part of any action that implements that offer – should it be accepted. However, these values are being regularly indirectly inferred from their willingness to pay for a life insurance policy. Here the policyholder is giving a value as to how much they need to be compensated if they lost it, involuntarily. One could argue that death due to complications from the COVID-19 infection could be classified as, ‘involuntary’.
Currently, in most countries in the world, the non-age discriminatory approach to fighting the war against the virus appears to have the full support of the younger population. But this support of government actions may change if the populace is only drip-fed information and policy; with no clear indication as to how long they would need to be under the current restrictive environment.
If the mood of the public turns; especially if the population is given no indication as to how long they will need to be partially or fully ‘locked-up’ without income or access to their lifestyle, then these minor rumblings can turn into disquiet on the streets, rampant flouting of laws, and ultimately anarchy.
To prevent this, in countries like Australia, the market economy must be preserved, and a recession or depression avoided. The key question on everyone’s minds is ‘how long before a semblance of normality returns?”
For this we need sound economic modelling.
Economic Modelling (To Fight War No.2)
In market economies, governments mostly keep out of the way. They support international trade, global supply lines and efficient and lean manufacturing. The banking system supports this free market system, and Central Banks only get involved in monetary policy at the macro level. The currencies are floated, with settlement in an internationally accepted currency.
This was Australia, just a month ago. In the last three weeks, under a national State of Emergency, the Australian federal government has taken full control of the everyday life of all its citizens; and has promised to spend many billions of dollars to keep the economy in ‘hibernation’ for the next six months. The theory is that those that go into hibernation will re-emerge when the worst is over, suggesting that things will almost be back to normal within 6 months.
But how many billions will be required? We are being drip-fed this information, and there is very little economic modelling that is readily available for us to get a sense of the scale. Governments may be having more information, but they are not telling us.
The government has still not released the pandemic modelling the Australian Health Protection Committee has used to recommend its escalating social distancing measures. Also, we are not being told how we will eventually pay for all this.
In a paper published just a month ago (in February), McKibbin & Fernando (2020) explore seven different scenarios of how COVID-19 might evolve in the coming year; and the impacts of these scenarios on macroeconomic outcomes and financial markets.[xiii]
Very sophisticated economic modelling is undertaken to ascertain the global impacts relative to the impact the virus had caused in China. In their worst-case scenario of a severe (but temporary) global outbreak of the virus, they estimated that the Australia GDP loss in Australia due to COVID-19 would be US$ 103 Billion (AUD166 Billion).[xiv]
A more recent Economic Impact model was published by PricewaterhouseCoopers (Thorpe & Loughridge, 2020).[xv] The approach adopted was conceptually similar to that employed by the Commonwealth Treasury in its modelling of the SARS outbreak of 2002-03.[xvi] The authors used a model of the global economy – the Global Trade Analysis (GTAP) model – which is a multi-region global, multisector, computable general equilibrium (CGE) model.[xvii]
In the model they assumed impacts over the next 12 months addressing:
- Labour input
- Capital productivity
- Government spending
- Technological shocks
- Private consumption
The PwC model estimates that over a year, a coronavirus pandemic could reduce Australia’s GDP by $34.2 billion; and that Australia’s household consumption will decline by A$37.9 billion over the forecast year. We now know that this is widely inaccurate; with the Australian Prime Minister announcing on March 30, a $130 Billion lifeline for millions of workers for 6-months.
Asking Australians to put the economy into ‘hibernation’ for 6 months gives the sense that its Federal and State leaders are imposing order on what could be a chaotic situation. However, trying to model economic impacts of this global pandemic based on the experience gained from past virus outbreaks is clearly fruitless, and indicates that nobody really knows what they are dealing with, and when it will be over, and how, if ever will we pay for it.
In essence, Australia is flying blind.
The Case for a Targeted Approach
By placing draconian social distancing measures on all its citizens, some governments, including in the USA, UK and Australia, are using a ‘shotgun’ approach to the pandemic. What is needed is a targeted ‘sharpshooter’ approach in protecting the most vulnerable, whilst keeping the economy running. [xviii] These governments need to follow the Taiwan, South Korea and Singapore models of keeping the economy open, subject to stringent safety rules and combined with extensive testing, contact tracing and detailed people tracking. This may be challenging in more democratic societies who inherently value their freedoms and place lower importance on Government directives or authoritarian approaches.
A strong case has been made here that this ‘suppression’ strategy of the Australian Government for 6-months is excessive, and that there will be very little change in patient outcomes if the government spends $12 Billion on providing a full capacity number of ICU Beds for 3-months to get over the peak. This will not only significantly reduce patient deaths; but also save the $65 Billion if it opens the economy with such a targeted suppression approach and contact tracing.
In terms of contact tracing and detailed people tracking, we can use our phones as tracking devices. Already there are articles that location and personal data of individuals who have tested positive to COVID-19 be shared with governments by the likes of Facebook and Google. In Singapore, their tracing team has used CCTV to find people; and in recent days a voluntary contact-tracing phone app using wireless Bluetooth technology called TraceTogether has been launched to allow local to quickly track down those who may have within two meters of a diagnosed case for at least half-an-hour.
However, from my own experience in consulting to large telecommunication companies, I am aware that one does not need smartphones or Bluetooth apps to do such tacking. The location of anyone with a mobile phone (even a non-smart Nokia or Blackberry) can be picked up using the network of ‘Base Transmission Stations’. This data is often stored by the phone company for a limited period. In the hands of an expert with adequate security clearance, the distances between phones, and therefore those carrying them, can be obtained with pinpoint precision.
Governments need to think outside the box to get our economy going again by exploring novel ways to prevent the health care system from being overwhelmed in the ‘peak’ period; whilst still ensuring a workable market economy.
The cure need not be worse than the problem if the medicine is properly administered.
References
[i] The Economist (2020), “The world gets ready Covid-19 is now in 50 countries, and things will get worse, Economist, Briefing, Feb 29, https://www.economist.com/briefing/2020/02/29/covid-19-is-now-in-50-countries-and-things-will-get-worse
[ii] Tim Churches and Louisa Jorm (2020), “We can ‘shrink’ the COVID-19 curve, rather than just flatten it”, University of NSW, https://newsroom.unsw.edu.au/news/health/we-can-shrink-covid-19-curve-rather-just-flatten-it
[iii] Neil M Ferguson, et.al., (2020), “Impact of non-pharmaceutical interventions (NPIs) to reduce COVID19 mortality and healthcare demand”, WHO Collaborating Centre for Infectious Disease Modelling, Imperial College London. March 16, p. 1-20. https://www.imperial.ac.uk/media/imperial-college/medicine/sph/ide/gida-fellowships/Imperial-College-COVID19-NPI-modelling-16-03-2020.pdf
[iv] Peter Hicks, Sue Huckson, Emma Fenney, Isobel Leggett, David Pilcher and Edward Litton (2019), “The financial cost of intensive care in Australia: a multicentre registry study”, The Medical Journal of Australia, Research Letter, 9 September, Vol 211, No. 7. https://www.mja.com.au/journal/2019/211/7/financial-cost-intensive-care-australia-multicentre-registry-study
[v] Paul Franks & Peter M Nilsson (2020), “Life is carrying on as normal in Sweden – scientists explain the controversial approach”, The Conversation, 29 March, https://www.weforum.org/agenda/2020/03/sweden-under-fire-for-relaxed-coronavirus-approach-here-s-the-science-behind-it/
[vi] This calculation of ICU Bed costs, capital expenditure, organisational overhead costs, and equipment costs were not included.
[vii] This assumes that there are adequate health care professionals to cover the surge in beds.
[viii] Alan Collins and Adam Cox (2020), “Coronavirus: why lockdown may cost young lives over time”, The Conversation, March 26, https://theconversation.com/coronavirus-why-lockdown-may-cost-young-lives-over-time-134580
[ix] David L. Chandler (2020), “MIT-based team works on rapid deployment of open-source, low-cost ventilator”, MIT News Office, March 26, http://news.mit.edu/2020/ventilator-covid-deployment-open-source-low-cost-0326
[x] Liam Mannix (2020), “Australia’s first virtual hospital rolls out for COVID-19 patients”, The Age, News, Monday, March 29, p.11.
[xi] Dylan Scott (2020), “The Covid-19 risks for different age groups, explained”, Vox.com https://www.vox.com/2020/3/23/21190033/coronavirus-covid-19-deaths-by-age
[xii] Dylan Scott (2020), op cit.
[xiii] Warwick McKibbin & Roshen Fernando (2020) The Global Macroeconomic Impacts of COVID-19: Seven Scenarios”, CAMA Working Paper 19/2020, Crawford School of Public Policy, Australian National University, February. pp. 1-43.
[xiv] Australia’s GDP in 2019 was A$1.89 trillion
[xv] Jeremy Thorpe & James Loughridge (2020), The Possible Economic Consequences of a Novel Coronavirus (COVID-19) Pandemic”, Australia Matters, PricewaterhouseCoopers, March, pp 1-10.
[xvi] Commonwealth Treasury of Australia (2003), ‘The economic impact of Severe Acute RespiratorySyndrome (SARS)’, Economic Roundup, Winter, pp.43-60
[xvii] Corong, Hertel,. McDougall, Tsigas and Van der Mensbrugghe, Dominique (2107), ‘The Standard GTAP Model, Version 7’ 2(1) Journal of Global Economic Analysis, Volume 1-119.
[xviii] Particular preventative care must be provided in age-care homes, especially in western countries, where societal norms are such that older citizens do not usually live with their children.


Pingback: Funding Manufacturing Post COVID-19: A National Security Issue – CMA Australia On Target
Pingback: Funding Manufacturing Post COVID-19: A National Security Issue - Academy of Finance
Pingback: Australian Government’s COVID-19 Responses Based on Dodgy Modelling – A $65b Saving Is Possible – CMA Australia